 As Labour Day rolls around, I’ve been giving some thought to the two-and-half years I spent as a worker rep on Athabasca University’s joint health and safety committee (JHSC). While the employer had long had a JHSC, it was effectively non-functional until the government changed the rules to make JHSCs mandatory (which better empowered the worker reps).
As Labour Day rolls around, I’ve been giving some thought to the two-and-half years I spent as a worker rep on Athabasca University’s joint health and safety committee (JHSC). While the employer had long had a JHSC, it was effectively non-functional until the government changed the rules to make JHSCs mandatory (which better empowered the worker reps).
Early COVID response
When I raised the issue of COVID with the committee in early 2020 (before the pandemic arrived in Alberta), I basically got laughed out of the room by the employer reps and no action was taken. Some worker reps had their union pressure the employer to act (including transitioning to working from home, suspending travel and eliminating the sick note requirement). It also published a blog to alert workers to things they could do in the absence of an institutional response.
This approach is pretty in keeping with what we know about the most effective tactics worker reps can adopt to get achieve change through JHSCs (which can only make recommendations). The employer basically adopted the union’s recommendations a week later and AU transitioned to working from home.
Transitioning to Working from Home
This transition to working from home was not without its difficulties, including several OHS issues. These included serious ergonomic issues as staff were now working from wherever they could find space in their homes and many were using small laptop computers, sometimes with inadequate internet service. These issues lingered unattended for months.
There was also a significant workload issue as certain institutional processes were not easily adaptable to online delivery coupled with a huge surge in enrollments. These issues were essentially left to individual staff members to sort out and numerous staff reported very high working hours and rapid burnout.
Workload problems were compounded by the departure of 53 staff (5% or so) who had taken a buyout option, overall heightened stress due to the pandemic disruption (including school and daycare closures), and social isolation. All of these issues were left unattended for long periods of time.
The union continued to work with its members to identify issues the university would need to address when it re-opened. As it happens, AU did not ever return to in-person working and the university used the two-years to slowly advance its plan to eliminate on-site work entirely (including closing two of its course campuses and classifying most of its staff at home-based workers).
Aerosol spread and hazard protocols
During COVID it became clear that the main method of transmission of the virus was through aerosol spread (although transmission by touching and droplets was also possible). Very loosely speaking, aerosol spread basically means the virus hitches a ride from an infected person to others on water molecules that an infected person exhales. The molecules with the virus can then be inhaled by people in the surrounding area. If you inhale enough of the virus, you too can become infected. This is a bigger issue in enclosed spaces than outdoors because virus-laden molecules typically dissipate faster and further outdoors.
The easiest way to understand aerosol spread is to think of it as farting. When you fart, the smelly particles are initially concentrated near the “farter”. But, overtime, the particles spread throughout the room and everyone can smell it. Simply being 6 feet apart (a common COVID protocol to prevent droplet spread from a sneeze or cough) does not protect from aerosol spread. If Travis “farts” and Stacey is 8 feet away across the room, Stacey is eventually going to smell it, right? Same idea with aerosol spread of COVID. The longer you are in close proximity to someone “farting” COVID, the higher the concentration of the virus-laden molecules, and the greater the risk of contracting COVID.
For this reason, effective hazard-control protocols for COVID include not working in enclosed spaces with other people. No exposure means no risk of transmission. If you are sharing spaces, other controls include enhanced ventilation (to reduce the concentration of the virus in the air) and masking. Masking prevents the virus from getting into the air (concentration is lower). And it also prevents someone from inhaling as many particles (which reduces the risk of catching COVID). Vaccination does not seem to control spread very much with Omnicron (so it is not really an effective control strategy); its primary value seems to be reduced severity of the disease.
Re-opening and COVID protocols
In September of 2021, government changes that gutted the effectiveness of JHSCs came into effect. You could literally see the energy go out of the JHSC as the tools the worker members used to keep the employer attentive to its OHS obligations effectively disappeared (e.g., there is no longer any requirement for workplace inspections).
In February of 2022, Minister of Advanced Education Demetrios Nicolaides directed all PSEs to end masking and vaccination protections. Directing post-secondary institutions to end mandatory masking eliminated one of the most effective controls on COVID transmission and placed post-secondary workers at risk of COVID. It also forced institutions to violate the OHS Act because they were no longer controlling workers’ exposure to COVID to the degree reasonably practicable. The Minister of Advanced Education has no authority to direct PSEs to act in this way or to waive the OHS obligations.
In May of 2022, Athabasca University altered its COVID protocols (presumably in response to the Minister’s direction). While most staff were expected to continue working from home due to the danger of infection, those staff who were on campus were no longer required to wear masks. This announcement basically says “it is too dangerous for you to come to work but, if you are onsite, don’t worry about wearing a mask”. This contradiction was so stark and evident that staff openly mocked it. It also dramatically increased the risk of aerosol transmission of COVID in the workplace.
The university’s Joint Health and Safety Committee was not consulted about this change. A review of Athabasca University’s hazard assessment revealed no consideration of aerosol transmission or controls. When this was brought to the university’s attention with a request to reinstate masking on campus, these concerns were dismissed and COVID control were further relaxed!
OHS Complaint and Inaction
Canada’s OHS system makes workers and employers jointly responsible for identifying and controlling hazards (the internal responsibility system). When this system fails, workers can file a complaint with government OHS inspectors (the external responsibility system). The existence of government oversight reflects that disputes about hazard identification and control can arise, sometimes via an innocent error and sometimes via a deliberate decision by the employer.
As worker co-chair, I filed an OHS complaint about the lack of controls around the aerosol spread of COVID (this is is how the system works). OHS investigated (without any discussion with workers) and declined to take action.
When I finally got to speak with the officer to find out what she’d decided (because there is no report-back system and you have to say certain magical words to get the officer to call you back), her explanation of inaction was:
- The employer did not identify aerosol spread on its hazard assessment and she could not force them to add it on, and
- She could not direct the employer to implement masking (which was explicitly noted in my complaint was NOT my request—I just wanted direction to the employer to develop a control strategy) in the absence of direction by the Chief Medical Officer of Health (CMOH).
- An employer cannot evade controlling a hazard simply by leaving it off a hazard assessment. Allowing this kind of evasion opens the door to employers ignoring all hazards by simply leaving them off the hazard assessment (like come on!). The OHS officer could well have identified the hazard the employer missed and directed the employer to develop a control strategy (which was my explicit request).
- The presence or absence of masking guidelines by the CMOH does not limit the ability of OHS officers to direct employer to develop a control strategy for a hazard. Masking is the obvious control, but the employer could also have improved ventilation or prohibited shared spaces. What is likely going on here is that OHS officers have been directed (or perceive themselves to be directed) not to require employers to implement control for the aerosol spread of COVID because of the government’s decision to let’er rip.
- The assertion that being six feet apart was an adequate control confuses controls for droplet spread with controls for aerosol spread. I could not have been clearer about this in my complaint. This raises questions about competence in my view.
- The absence of many workers working in close proximity is basically saying “well, not too many workers are at risk…”. The OHS Act and Code does not contain a threshold of injury or death that is required before an employer must take action.
Surprise Re-opening
Over the summer of 2022, AU embroiled itself in a stupid and public fight with the provincial government of AU’s long-pterm efforts to reduce the number of jobs in the local community. As a part of AU’s efforts to resolve this dispute (which imperiled institutional funding), AU announced on August 30 that the remaining two campuses would be open effective September 6.
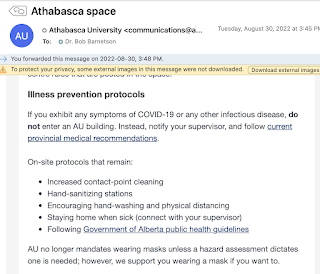
As part of the surprise re-opening announcement, new COVID protocols were announced. Basically, they amount to extra cleaning (to address touch spread) and staying home when sick, which is ineffective since (1) COVID carriers are contagious before being symptomatic, and (2) many COVID carriers are asymptomatic. There are no controls for droplet or aerosol spread. Staff are allowed to voluntarily wear masks if they want:
AU no longer mandates wearing masks unless a hazard assessment dictates one is needed; however, we support you wearing a mask if you want to.This approach individualizes responsibility for preventing the spread of COVID. It is just straight-up negligent because of the lack of droplet and aerosol controls. But the absence of any will by the government to enforce the OHS law means the employer can basically do whatever it wants.
Staff have little recourse except to (1) wear their own mask (the efficacy of which will be reduced because masking works best when everyone does it) or (2) try to avoid working on site if possible. Work refusals are unlikely to be effective since OHS has already refused to address aerosol spread and workers can choose to wear their own mask.
The only real option is for one of AU’s unions to file a grievance that AU is failing to address its obligation to provide a safe and healthy workplace under the OHS Act. That will take literally years to reach resolution and AU will likely use the OHS officer’s decision not to issue an order and a defence. Another option is for the unions to organize some kind of illegal walk out (an outcome that I judge to be unlikely).
Upshot
The recent changes to the OHS Act and Code have rendered JHSCs largely useless (which was likely the intent). The government’s political decision to eliminate COVID protections have also rendered the external OHS system ineffective. Together, these factors will create a significant amount of unnecessary ill health (potentially with lifelong consequences). As an OHS researcher and practitioner, I gotta say, this just makes me despair and very happy that I'm close to retirement.
-- Bob Barnetson
No comments:
Post a Comment